What is Obsessive Compulsive Disorder?

Obsessive-compulsive disorder (OCD) is a mental health condition characterized by intrusive thoughts and repetitive behaviors. People with OCD often feel driven to perform certain rituals or behaviors in order to prevent anxiety-related thoughts from entering their mind. This can be extremely challenging, and takes up a lot of time, as many of the behaviors are very time-consuming and inconvenient. If you, a family member, or someone you know suffers from OCD thoughts, read on for information on its signs and symptoms, as well as treatments that may help.
We hope that after reading this article, you will have a better insight into what is obsessive compulsive disorder.
What is obsessive-compulsive disorder?
A diagnosis of OCD will be given when someone has both obsessive thoughts and compulsive behaviours. When someone with OCD has unwanted thoughts, they feel like they need to do something to reduce this tension. The urge could be to do something verbal or physical, like asking for reassurance or washing your hands, or overthinking something endlessly.
These thoughts and behaviors can be very disturbing, but they’re not usually harmful. For example, a person with OCD may be preoccupied with thoughts or images that they can’t control. These thoughts or images may trigger an intense fear or anxiety in the sufferer, but they don’t usually lead to the feared result.
What Causes OCD?
The traditional view is that OCD is an anxiety disorder. The symptoms get worse with increased stress, but there are also hints that it may be a kind of movement disorder rather than a problem caused by anxiety.
This is important because if OCD is an anxiety disorder, then it will be treated by standard anxiety treatments, which are generally antidepressants or cognitive behavioral therapy.
But if it is a movement disorder, then we would not expect anxiety treatments to cure it. Mostly they do not cure the condition. However, my experience is that some antidepressants, such as paroxetine, can help, and they do seem to reduce the rituals and checking behavior in many patients. This is often enough to make life more tolerable.
OCD, Tic Disorders and Tourettes
Instead of unusual movements, OCD is defined by unusual behaviours. Compulsions are repetitive and excessive behaviors that a person feels compelled to do because of unwanted and uncontrollable thoughts. Performing the compulsion temporarily stops the repetitive thoughts, which are called “obsessions.”
In the first editions of the statistical manual of mental disorders DSM and the International Classification of Diseases (ICD), OCD was put into the category of anxiety disorders.
Disorders like Tourette Disorder (TD) are marked by repeated movements, while obsessive–compulsive disorder is marked by repeated behaviors.
In tics, repetitive movements are caused by an urge to move or do something. In OCD, repetitive behaviour is caused by a set of thoughts that urge the sufferer to do something. You can see how they are similar.
And in some chronic tic disorders, like Tourette syndrome (TD), complex, stereotyped movements can look like OCD, and early-onset OCD is often linked to complex tics.
Despite the differences between tics and OCD, the border is not so distinct, as the two diseases are commonly connected, and some OC symptoms, such as repetitive rituals of touching and compulsive symmetry, can even look like complicated tics. In addition, in patients with TD, it is believed that 60% also suffer from OCD, whereas roughly 30% of individuals suffering from OCD also display tics.
Risk Factors
The exact cause of obsessive-compulsive disorder is unknown. There are many risk factors that can lead to its development. Some of the risk factors include a family history of OCD, being female, and having a personality that is prone to feelings of anxiety or stress.
After a streptococcal (strep) infection, like strep throat or scarlet fever, obsessive-compulsive disorder (OCD), tic disorder, or both can appear out of nowhere. When you have strep throat, your OCD or tic symptoms get worse suddenly. In kids, this concept is a called “autoimmune neuropsychiatric disorders in children caused by streptococcal infection” (PANDAS).
There is an association between OCD and substance abuse. The reason for this is not clear, but it usually emerges in early adulthood.
For example, 70% of people with OCD reported showing signs of behavioural addiction. People with OCD were more likely to be addicted to the Internet than people without OCD, 29.3% versus 3.1%.
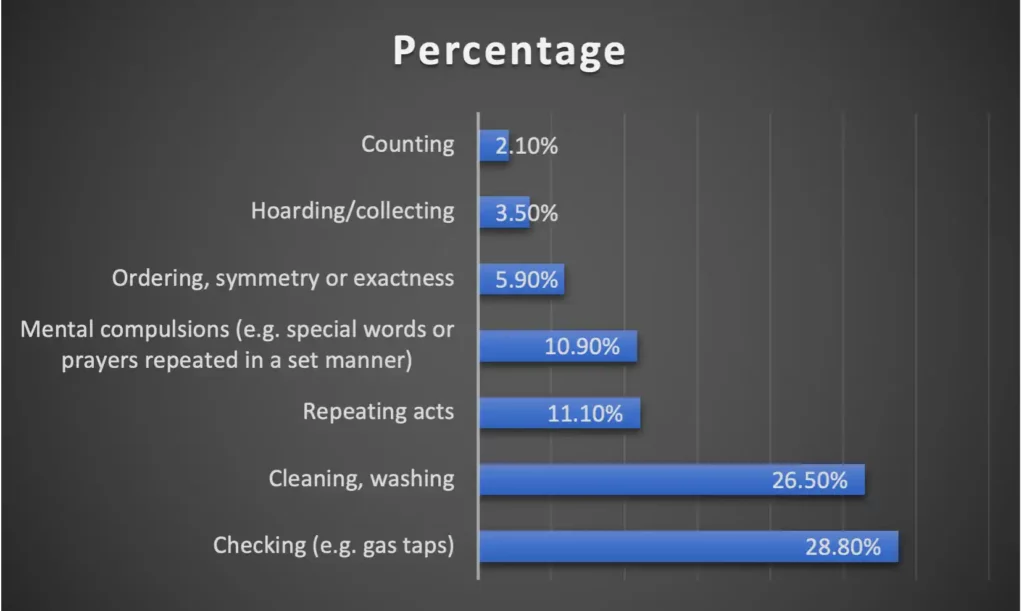
What Are The 4 Types of OCD?
OCD can be roughly categorized according to the type of preoccupation that causes the most problems. These are based on the theme of the obsessive thinking
Contamination Worries
Some people who have OCD are preoccupied with cleanliness and have a phobia of germs. They wash their hands until they are sore, clean the house beyond reason, avoid any sources of imagined (or real) disease.
Perfection Worries
Rather than an environmental phobia as with the contamination above, this may be related to feelings that the sufferer will be judged if things are not perfect. This has become internalised until the self is the main critic rather than others. Other people will tell you that it’s good enough, but you just can’t leave it. This drives you to exhaustion and anxiety.
Doubt or Harm Worries
This can focus on concerns that you might harm others, for example your child, or by poisoning family with your cooking — I’ve seen both of these commonly. Or that you might harm yourself by throwing yourself in front of a car or off a bridge. In fact, the anxiety caused by the very idea of these means that you will never do them.
Forbidden or Taboo Thoughts
These kind of obsessive thoughts are very difficult to disclose, and perhaps you don’t need to disclose them. They are usually sexual or violent and focus on harming people you absolutely shouldn’t harm, like killing your mother or your son. It’s different from the above because it’s not about killing them by accident, but about wanting to kill them deliberately.
It’s the same with sexual thoughts. You might have intrusive thoughts of having sexual relations with a family member or a child.
While, it is extremely unlikely, and I want to put another extremely in there — extremely, extremely unlikely that you will act these out, just to keep everyone safe, if you feel either violent or sexual thoughts are becoming overwhelming you need to seek help from a mental health professional.
I see a number of people who are very worried that they have this kind of idea and I try to explain it in this way:
Everyday we have a million thoughts, about the weather, about our shirt, about cake, about what we did last summer and we don’t remember 99.999% of them. They come and they go, not leaving much of a trace.
But some thoughts, chiefly violent and sexual ones, because they are so taboo are charged up. We might suddenly have a thought of this kind and then panic and by panicking we charge it up.
It’s like if I say to you: Please don’t think of white teddy bears. You immediately think of a white teddy bear and the more you try not to think of it, the harder it is, even though you may never have thought about a white teddy bear in your life before.
Imagine if a taboo thought pops into your mind? Your efforts to push it away charge it up so much that it keeps on coming back and back.
In this section, I’m not suggesting a cure for these, I’m merely explaining how they happen and that they are a mental event, not a sign that you are depraved and evil. You’re not.
What are 3 major symptoms of obsessive compulsive disorder?
Obsessions
Obsessions are unwanted thoughts or images that can be extremely intrusive and disturbing. They are usually related to a person’s fear of contamination or violence. Often, people with OCD will have to repeat the same task repeatedly in order to make the thoughts go away. Thankfully, there is help available—medication and therapy can help conquer symptoms of OCD.
Violent Obsessions
These thoughts often take the form of violent images or impulses. These are usually experienced in a specific way, which might convince the sufferer that they are more than just thoughts. But they are not more than just thoughts, that is all they are.
You may have violent or sexual thoughts that go through your mind over and over again. But they’re just thoughts, and just because you have them doesn’t mean you’ll do anything about them. In fact it is very rare that a sufferer from OCD will act on an intrusive thought of violence.
An Obsession with Symmetry
Needing to have things balance or be in symmetry is common. Sufferers often avoid odd numbers and volume dials and other controls have to be set at even numbers, very often 4. Often there needs to be the same number of object on the right as on the left and balance is important.
You might to make sure all the labels on the cans in your cupboard face the same way.
Contamination Obsessions
Obsessions about germs, contamination and dirt are common among people with OCD. These thoughts can consume your life, leading to compulsive behaviors such as checking locks, cleaning excessively or washing hands a lot.
Treatment for contamination concerns typically involves cognitive behavior therapy (CBT), which helps you learn different ways of thinking about the obsession symptoms so that they no longer have control over you. By changing the way you think about these thoughts, CBT enables you to manage them in a more manageable way and live a normal life again.
Sexual Obsessions
Sexual obsessions are recurrent and thoughts about sex, violence, or other obscene topics. They can be experienced at any time and in any setting – even at work.
In rare and very distressing cases, these obsessive thoughts often bring with them a compulsion – for example, the need to repetitively touch oneself sexually or think about the sexual act itself. There is very low risk of the thought actually happening.
streptococcal infection
Checking Obsessions
Checking is one of the most common obsessions in OCD. It can be anything from counting to making sure objects are in their place. People with Checking obsessions worry that, whether on purpose or not, they will do something bad to themselves or others. This constant worry makes them anxious, so they do checking rituals to make sure nothing bad has happened or will happen.

Intrusive Thoughts
Intrusive thoughts are unwanted ideas that can come to us at any time and without warning. They’re almost always the same thought repeatedly, and they can be upsetting or even disturbing.
One of the most common kinds of unwanted thoughts is a worry about danger or safety. People often have these kinds of thoughts in the form of images. For example, they might imagine driving their car through a crowd of people, hurting or killing someone else, or imagining a loved one being hurt or killed. Many new mothers worry that something bad will happen to their child. Thoughts about God or sex that are not appropriate are also common.
These repetitive compulsive thoughts that play again and again create a tension until they are acted out. Though people break OCD into two: the repetitive obsessional thoughts and then the compulsions that arise from them (the mental act and the physical act) are actually part of a single process.
The anxiety felt by people until they act out the thought is like the open loop anxiety described in Zeigarnik Tension.
Read about Zeigarnik Tension
https://www.rightattitudes.com/2017/03/14/zeigarnik-effect/

Compulsions
Compulsions, or compulsive acts, are repeated, deliberate physical or mental actions that a person feels compelled to do according to their own strict rules or in a stereotypical way.
Most of the time, the person feels like they don’t want to do the act, but the strong, personal drive to do the act wins out. Most of the time, the main goal of compulsive behaviour is to get temporary relief from the anxiety caused by the obsession that came before it.
Common preoccupations in OCD include thoughts of germs, dirt, or violence. Compulsions in OCD can involve a variety of behaviors, such as counting, checking, touching, ordering, and repeating words or phrases aloud. Treatment for OCD typically involves medication and/or therapy sessions aimed at reducing the symptoms of the disorder. However, if obsessions and compulsions are causing significant distress or interfere with daily life, treatment may also involve cognitive-behavioral therapy.
Treating obsessive compulsive disorder
The following are the most common and helpful ways of treating OCD:
Exposure Response Prevention
People used to think that OCD couldn’t be treated because people with it didn’t respond well to traditional psychodynamic psychotherapy, medication, or behavioural interventions.
Exposure and Response Prevention, or ERP, is a therapy that helps you face your fears and let your obsessive thoughts happen without trying to “fix” them or “neutralise” them with compulsions.
Later studies showed that this method of exposure and response prevention (ERP) worked in both inpatient and outpatient settings, and that most patients saw a big improvement that lasted for many up to two years after treatment.
ERP has become the first line psychotherapy method used to help people with OCD.
Even though up to half of people achieve few or no symptoms after an initial treatment with ERP many people who go through the therapy will still have symptoms, and some will get no benefit at all.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6343408/
Medication
Selective Serotonin Reuptake Inhibitors are a group of pills that are recommended as a first step (SSRIs). These help the brain use its serotonin better. Serotonin is a chemical that is used in a lot of different ways. They can also help with low moods and depression, so you might hear them called anti-depressants as well as anti-obsessional.
These include
- Fluoxetine (trade name ‘Prozac’)
- Fluvoxamine (trade name ‘Faverin’)
- Sertraline (trade name ‘Lustral’)
- Paroxetine is sold under the name “Seroxat.”
- Citalopram (trade name ‘Cipramil’)
- Citalopram (trade name ‘Cipramil’)
Some older Tricyclic Antidepressants such as clomipramine are also licensed in the UK
As a general rule, therapy and medication together can be the best way to help people get better and stay better. In the end, many people want or need both.
While a social worker or psychologist or nurse can give therapy, a psychiatrist will be the one who prescribes this medication.
Psychological Therapies
The type of psychotherapy most common for the treatment of OCD is Cognitive-behavioral therapy (CBT). Cognitive behavioral therapy is a mental health treatment that aims to change the negative thought patterns that lead to obsessive-compulsive disorder symptoms.
CBT for OCD will nearly always focus on sessions of exposure and response prevention (ERP).
ERP is technically a behavioural therapy (that’s the B in the CBT) but it will be backed up with advice on thinking about the compulsions differently, or looking for the evidence behind the need to check to make things safe (and that’s the C in CBT).
People with OCD that isn’t too bad usually need 10 hours of therapy, with exercises to do at home in between sessions. If your condition is more severe, you may need more time to get better.
The downside of therapy is that the techniques you get taught become obsessions and rituals in their own right.
Some of the procedures employed in cognitive behavioural therapy to assist people confront their thoughts or control unpleasant emotions can become compulsive rituals.
Neurosurgical treatment
Deep Brain Stimulation
Deep Brain Stimulation (DBS), an advanced surgical treatment that uses electrical impulses.
Brain scans help locate the part of your brain that is causing the symptoms. Then doctors implant two electrodes into that area and they also implant a neurostimulator, a small device similar to a pacemaker, that delivers mild electrical signals. put the device near your collarbone.
Doctors then connect the electrodes, which carry the electrical current to the neurostimulator. This system lets themsend electrical signals to your brain, which helps with your OCD symptoms. Doctors use DBS for OCD patients when they are severely ill or other treatments have not worked. It is effective for about 60 percent of these patients. If you receive DBS, you will likely feel relief soon after the procedure. The effects are long-term. DBS patients can generally take less medication.
Bilateral cingulotomy
A Bilateral cingulotomy is a type of brain surgery that is considered a last resort for people with obsessive-compulsive disorder (OCD).
It is also used to treat major depression and sometimes chronic pain in people who haven’t gotten any relief from other therapies. This surgery will focus on two areas of the brain: The cingulate gyrus helps control pain and emotions. The frontal lobes, which do things like reason, control impulses, and judge,
For a bilateral cingulotomy, a targeted radiation device called a “gamma knife” is guided to the cingulate gyrus with the help of magnetic resonance imaging (MRI). There, the surgeon will cut or burn about half an inch to break the circuit. It takes about four days to get better after an operation.
Some people get headaches, feel sick, and throw up in the days after surgery. Some people may also have seizures after surgery, but this usually only happens to people who have had seizures before. Some people say they feel unmotivated after surgery, while others have trouble remembering things.
These are not common, but they are risks that people who want to have the surgery should think about.
Even though bilateral cingulotomy can help some people, it is not a cure for everyone. A 2016 review of clinical studies found that 41% of patients who had a bilateral cingulotomy had a positive response to the procedure, while 14% had short-term side effects and 5% had serious side effects.
Repetitive transcranial magnetic stimulation
Repetitive transcranial magnetic stimulation (rTMS) is a noninvasive way to stimulate nerve cells in the brain which is getting more and more attention as a way to treat different mental illnesses. More and more evidence is showing that rTMS can help people with obsessive–compulsive disorder (OCD).
In conclusion, rTMS shows promise as a new neurostimulation technique that can be used as part of a toolbox of psychiatric treatments for OCD. It is a non-invasive treatment and so is easier to tolerate.
Also, rTMS could be an option for people who can’t tolerate medication and don’t get much help from psychotherapy.
Despite encouraging first signs, we still don’t know how to best use rTMS or dTMS to improve the approach and get clinically useful results.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6029675/

What is OCD? Conclusion
Obsessive Compulsive Disorder is a distressing condition that has a serious impact on the sufferer’s quality of life and impairs their enjoyment or even ability to participate in work or social activities. For a long time it was thought to be untreatable but we are now seeing good results with medication and therapy, or a combination of both.
Many people will be helped by being prescribed SSRIs in combination with cognitive behavioral therapy that focuses on exposure response prevention.
Some new methods such as transcranial magnetic stimulation might be helpful for some people but results are mixed. A more invasive method, deep brain stimulation, involves surgery where electrodes are placed into the brain, and there are claims that it is helpful for 60% of patients, but as with all surgery, there are more risks involved than with non-invasive methods, and potentially higher costs.
A final hope is neurosugery where surgeons will cut certain pathways in the brain. This is not without side effects and neither is it guaranteed to be successful, but it will be something that is considered by patients who may have tried everything else and not obtained relief.
We hope you now have a better idea what is OCD. To begin your recovery start by contacting your healthcare provider to discuss diagnosis and treatment options.
Related Articles
Top 5 Herbs in Ayurveda for Treatment of OCD
Depression After Stopping Drinking
5 Most Effective Antidepressants for Anxiety and Depression (and 3 you should avoid)
How To Explain Anxiety To Someone